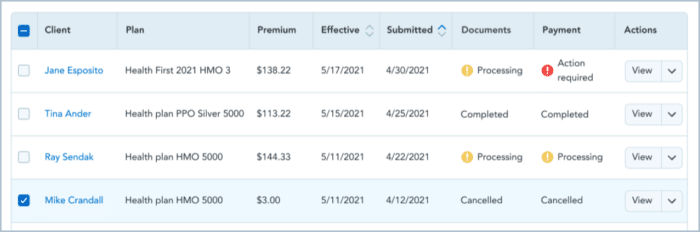
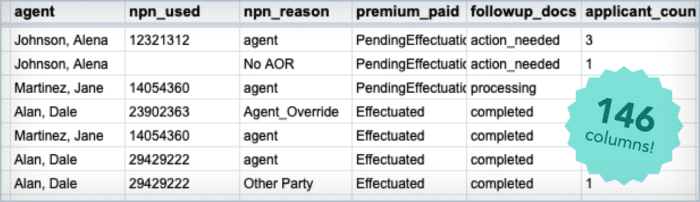
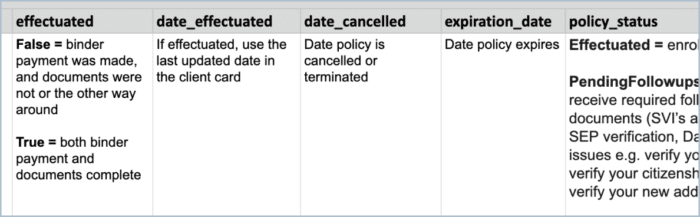
Consumers should Visit HealthCare.gov Beginning July 1 to see if they Qualify for New Financial Help.
As part of the American Rescue Plan (ARP) signed by President Biden,
the Centers for Medicare & Medicaid Services (CMS) is again lowering
the cost of health insurance and opening more pathways for Americans to
obtain affordable and comprehensive health coverage. Starting July 1,
2021, consumers who received or are approved to receive unemployment
compensation for any week beginning in 2021 may be able to find even
lower cost plans and save extra money on out-of-pocket expenses through
HealthCare.gov.
To take advantage of these additional savings, consumers who received
or have been approved for unemployment compensation in 2021 need to
visit HealthCare.gov to submit a new application or update their
existing application to maximize the savings they can get for the rest
of 2021. An average of three out of five eligible uninsured Americans
can access $0 plans after advance payments of tax credits and an average
of four out of five current HealthCare.gov consumers will be able to
find a plan for $10 or less per month after advance payments of tax
credits. CMS encourages current consumers who have received unemployment
income for any week beginning in 2021 to update their application and
enrollment between July 1 and August 15 to maximize the savings on their
Marketplace coverage for the rest of the year.
“The Biden-Harris Administration is focused on providing relief to
millions of families who need to access health insurance coverage
because they have been impacted by job losses or underemployment during
the pandemic,” said HHS Secretary Xavier Becerra. “The Administration
has made it easier than ever for Americans to enroll in an affordable,
comprehensive health insurance plans through HealthCare.gov thanks to
the increased financial assistance provided through the American Rescue
Plan. We encourage consumers who have received unemployment compensation
in 2021 to visit the Marketplace to see if they qualify to save money
on their health insurance premiums and out-of-pocket costs.”
“We are doing everything we can to remove financial barriers to
comprehensive health care,” said CMS Administrator Chiquita
Brooks-LaSure. “The American Rescue Plan provides consumers with
additional savings and will make coverage even more attainable for
those most in need. We welcome people who received unemployment benefits
in 2021 to check out their health coverage options on HealthCare.gov on
July 1.”
Additionally, as a result of the Biden-Harris Administration’s
Special Enrollment Period for the COVID-19 Public Health Emergency,
consumers can continue to apply for coverage, compare plan offerings, or
learn if they qualify for more affordable premiums by visiting
HealthCare.gov or CuidadoDeSalud.gov through August 15. Consumers can
view 2021 plans and prices and submit an application to see if they are
eligible for enrollment and financial assistance. If eligible, they can
enroll in a plan that best meets their needs. Current enrollees should
review their application, make any updates needed to their current
information, submit their application, and then select a new plan or
reselect their current plan to receive the increased savings under the
ARP.
Consumers can also call the Marketplace Call Center at
1-800-318-2596, which provides assistance in over 150 languages. TTY
users should call 1-855-889-4325. Consumers can also find a local
assister or agent/broker in their area: https://www.healthcare.gov/find-assistance/.
Consumers who live in a state with a Marketplace that operates its own
platform should visit their state Marketplace website or call center for
information on accessing these additional savings through their
State-based Marketplace.
(Original article published by CMS.Gov ‘https://www.cms.gov/newsroom/press-releases/american-rescue-plan-lowers-health-insurance-costs-americans-who-may-have-lost-their-job’)
Boost your book of business with ACA, Medicare, Life and more contracting!

Agility Producer Support
(866) 590-9771
support@enrollinsurance.com